Social determinants of health (SDOH) greatly affect people with complex chronic conditions. Innovista’s partnerships with community-based organizations help ease the burden of SDOH.
Serving the mental health needs of Texans poses a serious challenge for state practitioners, who struggle daily to work through access issues, largely due to lack of resources. For the second year in a row, Forbes Advisor ranked Texas the worst state in the country for mental healthcare, while also ranking it second highest in the number of uninsured adults with mental illness. Equally alarming, Texas ranked second highest in its percentage of youth with untreated depression. Given that Texas also has the third fewest mental health treatment centers in the nation (8.4 per 10,000 businesses), just making timely referrals
2024 was a banner year for value-based care. We discuss how this growth be sustained in 2025.
An overview of the best practices to code diabetes and diabetes-related health conditions and techniques to achieve Quality metrics.
Review the importance of regular breast cancer screenings, cervical cancer screenings, and other health evaluations crucial to proper risk adjustment for your practice.
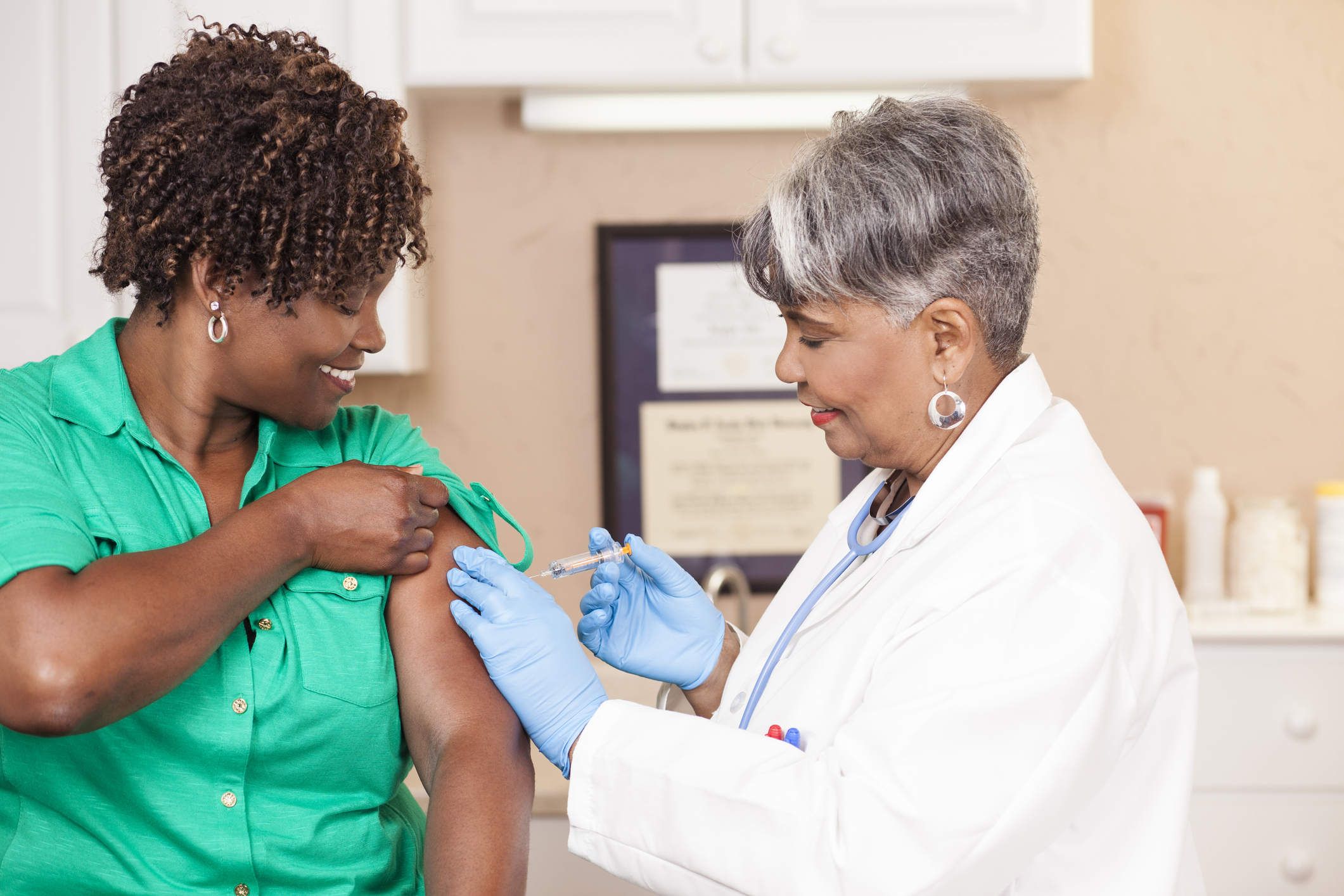
As temperatures drop, the leaves begin to change, and the scent of pumpkin spice fills the air. Plus, it’s a clear sign that flu season is just around the corner. Here’s what you need to know about flu season 2024, including who needs a vaccine, symptoms to watch out for, and practical tips to ensure that you and your family are prepared. What is the Flu? The flu, also called influenza, is a contagious respiratory virus. Its symptoms can be similar to the common cold, but they’re generally more severe. Unlike a cold, the flu can lead to serious complications,
Discover key actions to close gaps in patient care as we reach the end of the year – particularly scheduling AWVs and outstanding health screenings.
OAK BROOK, Ill., September 16, 2024 (Newswire.com) – Innovista Health welcomes Jigar Desai as its new President and Chief Executive Officer. Desai will lead the managed services organization as it further positions itself as the partner of choice to payers and independent physician groups in the design, management and administration of value-based care arrangements. Desai brings more than 20 years of managed care experience to Innovista Health. Previously, he held senior leadership roles at several Medicare-focused managed care organizations. Most recently, he served as executive chairman of a private equity-backed Medicare platform, where he implemented turnaround plans and led the acquisition of
Transitioning to value-based care (VBC) models may be daunting in the short term, but medical practices can expect to reap an abundance of long-term benefits for patients, staff, and their community. As VBC takes center stage as the future of healthcare, it is America’s physicians who are key to its successful adoption. As a physician leader, it is understandable that you are concerned about your practice’s readiness to make the shift. Leading efforts to set up a VBC model and pay arrangements is no small task. As payers drive VBC, providers are being thrust into the role of implementers, the
Review the importance of timely vaccinations for both children and adults and methods to encourage adherence to schedules.
Women’s health is in the spotlight this week as our nation celebrates Women’s Equality Day. Notably, August 26 marks the enactment of the 19th Amendment, which recognized a woman’s right to vote and gave voice to a wide range of health and other issues. While much has changed since this landmark decision in 1920, women still face significant healthcare challenges, not the least of which includes a higher incidence of misdiagnoses than their male counterparts. Diagnostic Inequality Of the 12 million adults who are misdiagnosed each year, women and racial/ethnic minorities are 20-30% more likely to experience a diagnostic error.
Diagnosing and managing respiratory conditions is critical to patient well-being. Learn methods to evaluate and address conditions such as pharyngitis, bronchitis, and COPD.
Learn how the conditions where people are born, live, learn, work, play, worship, and age impact the effectiveness of healthcare.
Discover the critical nature of Behavioral Health Screenings to identify and address Mental and Behavioral Disorders in your patient populations.
End-of-life care can be an uncomfortable topic. Early conversations about a patient’s wishes can help them avoid unwanted treatments. Learn more.
Walk through the reconciliation process of a patient ER visit, from admission to transition to home or secondary facilities.
Join us as we review the most common chronic conditions encountered while caring for older adults and the importance of discussing advanced care planning with patients and their caretakers.
Learn more about how improved Medication Adherence can reduce hospitalizations and healthcare dollars spent.
Data is a growing force in health care and will continue to be a driver now and in the future. Learn more about health care data trends to keep an eye on.
Patient engagement is one of the keys to success in value-based care. Discover strategies to boost your patient engagement.
Key information on streamlining and optimizing Annual Wellness Visits.
Good doctor/patient communication is paramount to a positive healthcare experience. These tips can help strengthen communication and relationships with patients.
Learn about new HCCs for 2024 and supplemental data, how this can affect your practice, and how to ensure proper coding practices.
V28 has changed capitation rates and risk adjustment methodologies in 2024. Discover how to implement V28 changes in your coding and practice.
Mutually beneficial value-based care contracts support both payer and provider efforts. Discover the key components of a good contract.
Management services organizations (MSOs) relieve administrative burdens and improve quality metrics for providers. But payers benefit too.
October 2023: Healthcare Quality Week; Tips to get your patients in for cancer screenings; and text messaging for better patient engagement.
Hospital readmission is costly and often leads to poor outcomes and even higher risk of mortality. Transitional care management aims to reduce readmission and improve patient outcomes.
CMS releases star ratings annually to help patients choose a Medicare Advantage plan that best meets their needs. Higher star ratings are important for providers and payers alike, but they’ve have been on the decline as of late. Is it possible to raise them?
Missed healthcare appointments lead to poor patient health. An effective text messaging campaign can reduce no-shows and improve annual screening rates.
CMS recently finalized policy updates for Medicare Advantage plans, which will significantly impact how practices manage risk and allocate resources. Here’s what to expect in 2024.
Many patients take multiple medicines to improve their health. Medication reconciliation helps providers track what patients use regularly.
Vaccines are critical to patients’ long-term health. Discover several ways providers can increase their immunization rates.
There’s a lot to consider before making the switch from fee-for-service to value-based care, but these 4 tips can help set a practice up for early success.
Physician burnout is a serious issue, affecting providers, patients and the healthcare system as a whole. Learn how value-based care can mitigate many of the factors that contribute to burnout.
Advanced care planning is difficult, but it’s essential to value-based care. These conversations benefit patients and providers alike. Learn how.
Medication nonadherence is a perpetual problem in healthcare. Learn how Innovista worked with a Houston area practice to improve their scores of this important triple-weighted measure.
Providers face some financial risk under value-based care. Risk adjustment coders safeguard payments by auditing files for accurate coding.
This case study illustrates the power of partnership between Innovista and a Chicago area practice in leveraging data to make better healthcare decisions.
Patients need the right care at the right cost. Utilization management nurses ensure members receive appropriate services based on evidence-based practices.
What do providers need to do to succeed in value-based care? There are several ways to foster financial success—but providers should prioritize four key plays to truly maximize incentives.
Pre-visit planning (or chart prep) helps create efficiencies within medical offices, ensuring smooth and seamless workflows. Learn how to put this useful technique into practice.
The healthcare system can be complex and confusing. Many patients need an advocate—a case manager—who can help them get the care they need.
In value-based care, teams of professionals work together to ensure patients are well cared for and practices meet benchmarks. Community health workers are key players in achieving these goals.
The emergency department is often a patient’s first choice for acute care, but it’s not always the best option. Providers can empower patients to choose alternative care settings using these tactics.
Seasonal scheduling is a way for physicians offices to adjust their schedules to make room for wellness exams during specific times of the year. Learn how to leverage this practice.
In value-based care, providers assume more financial risk than ever before using alternative payment models. What are the risks and rewards of these various payment models?
Emergency department visits are expensive and often avoidable. Mobile urgent care save practices money and improve health outcomes.
Uncertainty exists around whether value-based care offers a return on investment (ROI) for independent practices. But, it’s possible—with the right approach.
Social determinants of health (SDOH) impact healthcare for Medicaid patients. Community health worker/payer partnerships help mitigate SDOH and reduce unnecessary ED visits.
Patient data is vital to value-based care. However, managing it can be difficult. Working with a partner can help practices get a better return on their investment.
OAK BROOK, Ill., Aug. 30, 2022 /PRNewswire/ — Innovista Health (Innovista) today named Dr. Vikram Bakhru as its new chief executive officer. Bakhru is a practicing physician with more than 20 years of experience dedicated to the intersection of technology and the improvement of health outcomes for underserved populations. Dr. Bakhru most recently served as chief health officer for a managed Medicaid insurance company providing access to tech-enabled, quality care to the underserved. He also co-founded or served as a senior executive for several venture-backed health technology companies. “Stepping into this role, I am focused on having Innovista partner with care providers to leverage