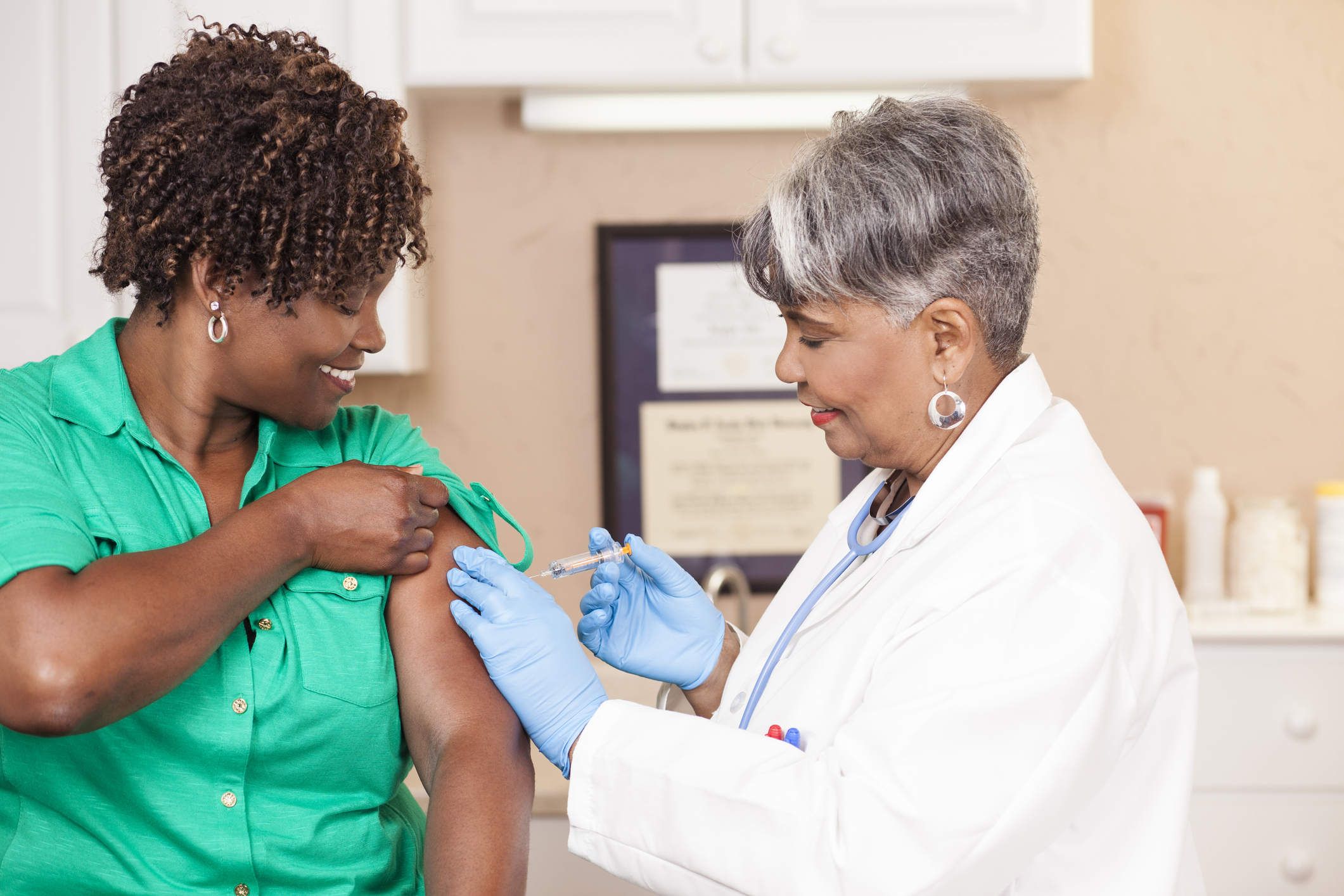
Patients can find navigating the healthcare industry confusing and overwhelming. They want good care, but knowing where to find it can prove challenging. The Centers for Medicare & Medicaid Services (CMS) makes finding good care easier with its Star Rating System.
Patients can rely on this five-star system to select a Medicare Advantage plan that best meets their health needs. But, according to Jonathan Owens, chief analytics officer at Innovista Health, practices should also pay close attention to this five-star rating system.
“For patients, choosing a health plan can be much like picking a restaurant when you’re out of town on business. When you’re away, you may open Google Maps, Yelp, or Open Table and see two restaurants—one with a two-star rating and one with four stars,” he says. “Between the two, you’re picking the four-star. It’s the same concept with Medicare Advantage plans.”
How are CMS Star Ratings Calculated?
Every year, CMS produces its Medicare Advantage health plan star ratings. One star is the lowest rating, and five stars is the highest. CMS bases these ratings on:
- Patient experience surveys
- Customer service (how well plans handle patient requests and appeals)
- Patient complaints about plans
- Chronic condition management
- Patient health during enrollment
“These ratings are a mixture of what patients report about their experience on the plan throughout the year and other information about the quality of care delivered,” Owens says. “It’s a measure of how easy it is for patients to access the benefits they need, as well as whether they received health services and medications.”
This system reviews 46 quality measures, including preventive screenings, medication reconciliation, medication adherence, and care coordination.
Why Do CMS Star Ratings Matter?
As a plan performance measurement, a star rating can impact patients and providers alike. Ratings can influence:
- Plan selection: Most patients have little experience in choosing a health plan. So, they rely on consumer reviews just like they would with other major purchases. Overall, patients will gravitate to plans that receive the most positive feedback from current and previous plan members.
- Reimbursement: CMS uses star ratings to allocate reimbursement. Higher-rated plans receive more money to use to pay for more patient benefits. Some plans also give larger payments to higher-performing providers who produce better patient outcomes.
“Doing this creates a two-way street. It starts with reimbursement coming from CMS that works its way through the plan to the provider,” Owens says. “Then, as the plan improves because of provider performance, benefits to the plan members increase, and star ratings improve.”
Being part of a highly rated plan potentially opens the door for providers to increase reimbursement, but it also offers other benefits.
For one, patients may be more likely to choose providers who align with higher-ranking plans. Also, since some plans incentivize providers who produce better patient outcomes, ratings can impact bottom line.
In addition, star ratings matter for physician practices because they increase opportunities to:
- Boost performance in other quality incentive programs.
- Expand patient base during special enrollment periods.
- Focus on preventive care, leading to early disease detection.
- Offer more chronic condition management programs.
Star Ratings are Dropping…But Why?
The number of Medicare Advantage plans with 4-plus star ratings decreased significantly between 2022 and 2023. Last year, 68% of plans reported a rating of over four stars. This year, just 51% secured the same score.
According to CMS, the average health plan rating fell from 4.37 stars in 2022 to 4.15 stars in 2023. Although this is a drop, there’s good news. The decline doesn’t mean health plans are deteriorating. Instead, it’s a re-set to pre-COVID-19 norms.
“During the pandemic, there was some relaxation on star ratings. The government recognized it would be a challenge to get patients to come in frequently, so they relaxed their requirements,” Owens explains. “What you’re seeing in 2023 is those relaxations going away. Ratings are coming back to reality and getting back to normal.”
Steps to Improve Star Ratings
Given how influential star ratings are for health plans and providers alike, it’s worth it for both parties to take proactive steps to improve them.
- Use quality modules: Most electronic medical record systems include quality modules to help practices track the process and outcomes measurements used in star ratings. For example, the gold standard for breast cancer screening is a mammogram every two years for female patients over age 40. A quality module can help you identify which patients haven’t yet received this service.
- Leverage plan benefits: Familiarize yourself with any benefits a plan provides to help patients access services. Some plans offer transportation to patients with no other way of getting to the doctor. Others offer prescription medication home delivery. Knowing what a plan offers can help keep patients out of the hospital and improve their overall quality of life.
- Monitor weighted measures: Every year, CMS focuses on various metrics to evaluate plans. Some, such as medication adherence, count more than others. To maximize your annual performance, assign dedicated staff members to track these measures, consider attaching incentives for providers to weighted measures, and update contracts with plans every year to reflect any CMS changes.
- Prioritize preventive services: Preventive services can improve overall patient well-being, leading to a high star rating. Encourage all patients—but especially those who are higher risk—to come in for screenings. Offer incentives to providers in your practice who conduct annual wellness visits and consider providing at-home visits for patients with transportation or mobility problems.
- Aim high: Be aware that score ranges for each star rating can change. CMS releases its estimated ranges at the beginning of the year. However, they may adjust those measurements at the end of the year based on the performance of all practices nationwide. Consequently, Owens says, try to outperform your own expectations on as many measures as possible.
“Set a target for your practice, and try to overshoot it a little bit,” he says. “CMS basically grades on a curve. So, be prepared to aim a little bit higher on some measures in case everyone else does really well.”
Partnering for a High Star Rating
To boost chances of achieving a high star rating, Owens recommends collaborating with a partner like Innovista. A partner can determine which patients need preventive services, coordinate patient care with providers, and even help providers enroll with a plan.
Ultimately, they relieve practices of the administrative burdens that might be a challenge to handle alone.
“Providers have been seeing less reimbursement for years, so they have less staff,” Owens says. “It’s a struggle to see patients all day plus have the energy and bandwidth to monitor your own star rating metrics. A partner can help practices become more effective as independent providers.”